Forty years ago, the AIDS epidemic broke out and gained recognition across the United States. A generation of gay men were victims of the disease and it took years before scientists understood how it was transmitted. Since then, there has been moderate progress — HIV transmission, as well as general STI/STD transmission, is mentioned in passing during sex education in high schools, condoms have become more accessible and, possibly the most importantPrEP, a drug used to prevent HIV transmission, was developed and distributed.
Human Immunodeficiency Virus, known commonly as HIV, is a sexually transmitted disease (as opposed to a sexually transmitted infection, such as chlamydia). Over time, HIV can develop into Acquired Immunodeficiency Syndrome (AIDS). Neither have a cure and can quickly turn fatal. For victims of AIDS, even a cold can become deadly because their immune system has no defense.
For years, and still a modern-day misconception, HIV/AIDS was called a “gay disease,” meaning the assumption was that only gay men could develop AIDS. The homophobia and stigma surrounding the disease persisted so long that it took four years after the first case in the United States for Ronald Reagan to make a statement. However, this myth is easily debunked today as women account for 28% of North Carolina’s HIV cases and 79% of those cases are transmitted through heterosexual contact. Currently, HIV/AIDS in North Carolina is a pervasive problem that persists 40 years after the epidemic began and affects populations across the state.
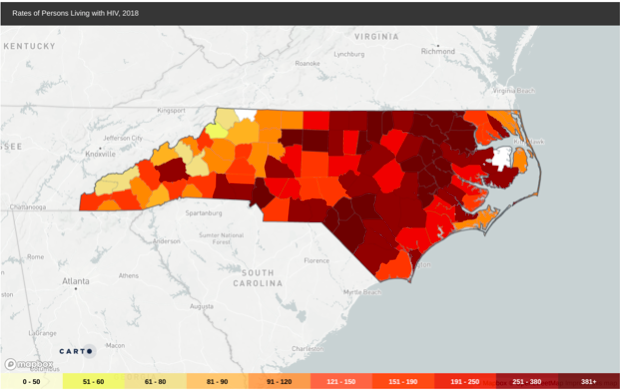
Despite the advancements in the past 40 years, rates of HIV have remained stagnant and the disease continues to affect pockets of North Carolina, with lower-income counties being the most affected. Using information from the AIDSVu Map, a project by Emory University’s School of Public Health, there were 31,864 people living with HIV in North Carolina in 2018. Given medical advancements, people with HIV are living longer, so the number of cases is unlikely to decrease sharply without a cure. However, the concerning factor is the number of new cases each year. After a sharp decrease in new cases in 2007, the level of new cases has remained consistent to 14 cases per 100,000, as of 2014.
It is important to remember that sexual education in the United States and North Carolina is inadequate when teaching people how STIs and STDs are transmitted and debunking myths surrounding HIV/AIDS, so it is likely these numbers are higher. In 2014, the CDC estimated that 4,900 people had untested HIV. Given the COVID-19 pandemic and the past 16 months, it is likely the number of undetected cases has grown in the past year since access to healthcare and testing was limited.
However, steps in North Carolina have been made to increase awareness, expand testing, and create better access to long-term treatment. In 2017, North Carolina developed a Continuum Care program for counties as part of the state’s Integrated HIV Prevention and Care Plan. The 133-page document tracks the number of HIV cases as of 2014, as well as demographic breakdowns, locations for treatment, and the funding they receive. Healthcare centers in each county are listed along with the goals to be addressed from the Continuum Care program such as testing, connecting patients to care, sex education, counseling. These additional programs, beyond just testing for positive cases, are necessary to contain and ultimately eradicate the disease. The first step is always prevention programs — educating others on how the disease is contracted, how viral it is, and the myths, such as which populations are vulnerable, surrounding HIV/AIDS. But there is so much myth and stigma surrounding the disease that can still persist after a diagnosis. Patients need to know how their life will change with HIV and how they can manage that change.
One predominant source of funding in North Carolina is the Ryan White HIV/AIDS Program. Not only does this program cover the standard testing and treatment, but it also has additional funding for dental healthcare, education training centers, and programs that focus on women and children with HIV. All 50 states receive at least some funding from the Ryan White Program. At the HIV Clinic closest to me in Wake County, the primary healthcare center is funded by the Ryan White Program. Since its inception 30 years ago, recipients and clinics associated with the Ryan White Program have made “what was once a deadly disease is now a manageable, chronic condition,” supporting the claim that HIV/AIDS treatment requires a multi-faceted treatment and prevention plan.
North Carolina’s HIV Prevention and Care Plan is set to phase out in 2021. Hopefully, a new document and plan will be published with updated statistics and future goals. Several factors affect HIV/AIDS treatment — region, access to healthcare, socio-economic status — and these issues will persist beyond this calendar year. The primary goal of the Plan was to establish the number of people undiagnosed and diagnosed with HIV in North Carolina and assess problems in the current care system. Beginning on page 58, the Plan lists different unmet needs that can affect treatment including access to transportation, food and nutritional care, mental health care, and bilingual services. These problems are later compounded into word bubbles, magnifying the biggest barriers such as “too few case managers,” “lack of evening and weekend hours,” and “lack of Medicaid coverage.” Many of these assessed needs conclude that there are not enough resources to meet the problem. Ideally, in a newly published plan, these needs are met and the prevention and long-term treatment of HIV/AIDS victims in North Carolina can begin.
 Claire Goray graduated from UNC-Chapel Hill in May 2020 with a major in American Studies and minors in Writing for the Screen & Stage and Sexuality Studies. Her interests include representation in film & media, examining the HIV/AIDS crisis, and studying the importance of historical monuments.
Claire Goray graduated from UNC-Chapel Hill in May 2020 with a major in American Studies and minors in Writing for the Screen & Stage and Sexuality Studies. Her interests include representation in film & media, examining the HIV/AIDS crisis, and studying the importance of historical monuments.
There are no comments
Add yours